"Have you ever felt a burning pain in your chest and wondered if it was just heartburn—or something more serious? What if that discomfort was a hiatal hernia, a condition that millions of people have but few truly understand?
In today's episode of The Gut Whisperer, we're pulling back the curtain on hiatal hernias—what they are, why they happen, and most importantly, how they can be treated. From simple lifestyle adjustments and powerful medications to advanced minimally invasive surgeries, we'll walk through the full spectrum of treatment options.
Whether you're living with acid reflux, struggling with swallowing, or just curious about how your stomach and diaphragm interact, this episode will give you the clarity and guidance you need.
Stay tuned—because understanding hiatal hernia symptoms could be the first step to real relief, better digestion, and a healthier future."
"Imagine a baby who spits up constantly, struggles with ear infections, and ends up needing ear tubes before his first birthday. As he grows, the spit-ups turn into sour burps, a chronic cough, and congestion that doctors mistake for asthma. By the time he's a teenager, he's battling chest pain, reflux during sports, and trouble swallowing.
This isn't just a random illness — it's a hiatal hernia. Today on The Gut Whisperers, we'll uncover how symptoms like these can start in infancy, evolve into adolescence, and what treatments — from lifestyle changes to surgery — can finally bring relief."
"This episode of The Gut Whisperers is proudly sponsored by two partners close to our mission.
First, Laguna by Andrés Spinetti — a breathtaking journey into the art and tradition of fly fishing in the Laguna Madre. More than a book, Laguna is a celebration of nature, storytelling, and culture, now showcased at the Texas State Capitol Library in Austin. You can get your copy today at carenowonline.com/products/laguna-pioner. It's a meaningful gift for anglers, nature lovers, and anyone who values artistry.
We're also sponsored by the Pediatric Gastroenterology Clinic of South Texas, where compassionate care meets advanced medicine. Located in Edinburg, Texas, our clinic is dedicated to helping children with digestive and nutritional conditions find answers and relief. From reflux and constipation to complex gastrointestinal disorders, we're here to guide families with expertise and empathy. To learn more, visit us at pgcost.com or call (956) 682-2244.
Together, these sponsors make The Gut Whisperers possible — and support our mission to bring trusted digestive health knowledge straight to you."
"Let me tell you about Daniel.
As a baby, Daniel seemed to struggle from the very beginning. He spit up after almost every feeding, cried with discomfort, and arched his back as if he were trying to escape the pain. His parents thought it was just colic. But then came the constant coughing and congestion. He always sounded stuffy, and ear infections became so frequent that by his first birthday, he needed ear tubes placed to help him hear and sleep better.
When Daniel became a toddler, the spit-ups didn't entirely go away. Instead, they turned into sour burps and small regurgitations after meals. He avoided eating certain foods, pushed his plate away, and his nights were restless. His mom often held him upright so he wouldn't cough or choke from acid that crept into his throat.
In elementary school, Daniel's symptoms shifted again. He complained of burning chest pain, sometimes telling his teacher his "heart hurt." Doctors thought it was asthma or anxiety because of his chronic cough and wheezing. However, the inhalers and antibiotics never solved the problem. He missed school due to recurring sinus congestion and upper respiratory infections that just wouldn't quit.
By the time Daniel reached adolescence, things became harder to ignore. During soccer practice, reflux burned his throat and made him cough uncontrollably. At meals, he sometimes felt food sticking in his chest, and he grew embarrassed when acid suddenly came back into his mouth. The lack of sleep, the constant cough, the congestion — it all took a toll on his confidence and energy.
Finally, after the proper tests were done, Daniel's family had answers: a hiatal hernia was the underlying issue all along. With an appropriate plan of treatment — dietary changes, medication, and eventually surgical repair — Daniel found relief. His coughing stopped, his infections lessened, and he was finally able to enjoy sports, meals, and school without pain holding him back.
Daniel's journey is not unusual. Many children start with ear infections, chronic cough, or congestion, and only later show the classic symptoms of reflux or chest pain. Recognizing the signs early can save years of discomfort — and help families find the proper treatment sooner."
"Request your 10 red flag of newborn in infants here"
Comprehensive Guide to Hiatal Hernia Treatments: Symptoms, Options, and Recovery
Looking for hiatal hernia treatments? This guide explores effective options, from lifestyle changes and medications to surgeries, to help you manage and relieve symptoms.
A hiatal hernia occurs when part of the stomach pushes up through the diaphragm. In this condition, the stomach moves from the abdominal cavity into the chest cavity through the opening in the diaphragm called the hiatus. The integrity of the abdominal cavity is an essential factor in the formation of a hiatal hernia, as weakened or compromised structures can allow the stomach to shift upward.
Introduction to Hiatus Hernia
A hiatus hernia, more commonly known as a hiatal hernia, occurs when part of your stomach pushes up through the opening in the diaphragm called the esophageal hiatus and into the chest cavity. This anatomical shift can disrupt the normal function of the lower esophageal sphincter, allowing stomach acid to flow back into the esophagus and triggering symptoms of acid reflux. As a result, individuals may experience hiatal hernia symptoms such as heartburn, chest pain, regurgitation, and difficulty swallowing.
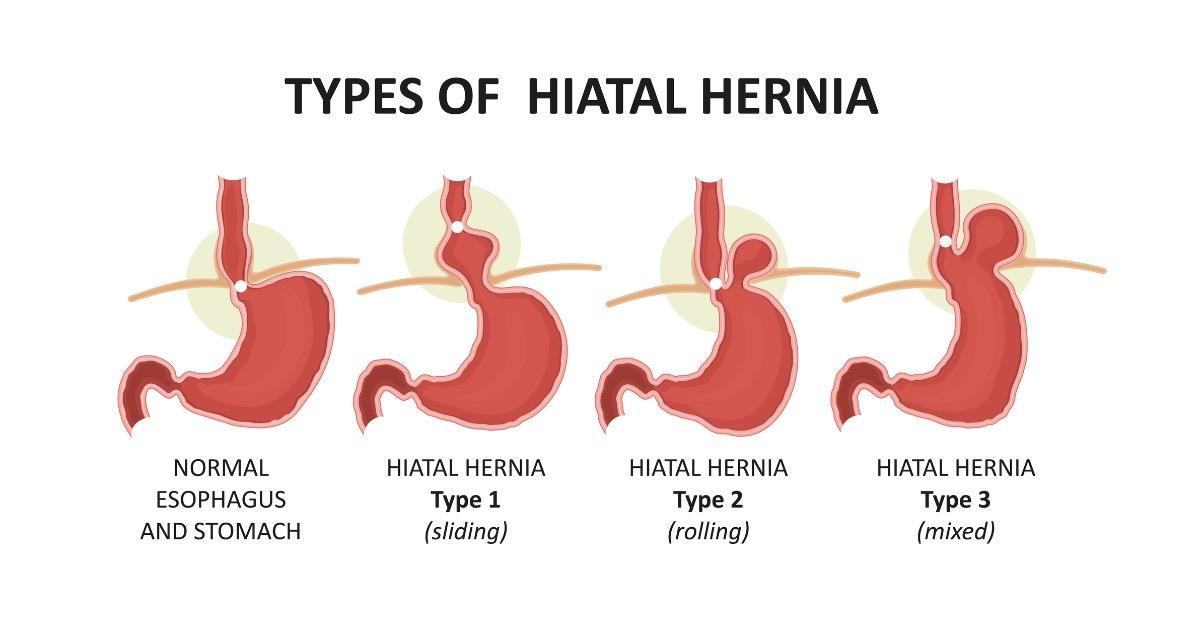
Hiatal hernias are classified into two main types: sliding hiatal hernia and paraesophageal hernia. A sliding hiatal hernia is the most common form, where the stomach slides up and down through the hiatus, often leading to gastroesophageal reflux disease (GERD) and related symptoms. In contrast, paraesophageal hernias occur when part of the stomach bulges alongside the esophagus through a weakness in the diaphragm. While sliding hiatal hernias are more likely to cause acid reflux, paraesophageal hernias can sometimes lead to more serious complications, such as gastric volvulus or compromised blood supply to the herniated stomach.
The severity of hiatal hernia symptoms can vary widely. Some people may have mild discomfort, while others experience persistent chest pain, swallowing problems, or even nausea and vomiting. If left untreated, a hiatal hernia can lead to complications like hernia recurrence, reflux disease, or, in rare cases, life-threatening emergencies.
Diagnosis of a hiatal hernia typically involves a combination of a physical exam, imaging tests such as a barium swallow, and procedures like upper endoscopy or esophageal manometry. These modern diagnosis methods help healthcare providers assess the size and type of hernia, as well as the impact on the digestive system.
Treatment for a hiatal hernia depends on the severity of symptoms and the type of hernia. Many people find symptom relief through dietary and lifestyle changes, such as maintaining a healthy weight, avoiding fatty or spicy foods, and elevating the head of the bed. Medications like proton pump inhibitors can help reduce acid production and manage GERD symptoms. For those with severe or persistent symptoms, or in cases of large or complicated hernias, surgical repair—often performed using minimally invasive laparoscopic surgery, such as laparoscopic Nissen fundoplication—may be recommended.
Early recognition and management of hiatal hernias are key to preventing complications and improving quality of life. With advances in diagnosis and treatment, most individuals can achieve effective symptom relief and return to normal activities.
Key Takeaways
Hiatal hernia symptoms often include heartburn, chest pain, and difficulty swallowing; recognizing these early can lead to more effective treatment.
Diagnosis typically involves methods such as barium swallow studies and high-resolution manometry, which ensure accurate identification of the condition.
Surgical options like laparoscopic Nissen fundoplication and non-surgical treatments, including lifestyle changes and medications, are vital for managing symptoms and preventing recurrence.
Understanding Hiatal Hernia Symptoms
Recognizing the symptoms of a hiatal hernia is the first step towards effective treatment. Common symptoms include:
Heartburn
Belching
Chest pain
Trouble swallowing
A general feeling of fatigue
These symptoms are often aggravated by the backward flow of stomach acid into the esophagus, which is a hallmark of hiatal hernias. This acid reflux can lead to persistent discomfort and even damage the esophageal lining over time.
The pain associated with a hiatal hernia can be severe, manifesting as sharp chest or abdominal pain, often mistaken for conditions like heart disease. Hiatal hernia can present with the same symptoms as other gastrointestinal or cardiac conditions, such as heartburn or angina, making diagnosis challenging. Larger hiatal hernias can lead to more serious symptoms, such as vomiting blood or passing black stools, both of which indicate severe internal bleeding and require immediate medical attention. Paying close attention to these symptoms and seeking medical advice if they persist or worsen is crucial.
In some cases, a hiatal hernia can cause chronic gastroesophageal reflux disease (GERD), characterized by frequent acid reflux, chest pain, and swallowing difficulties. The constant presence of stomach acid in the esophagus can lead to significant discomfort and disrupt daily activities. Understanding and recognizing these symptoms early can lead to more effective management and treatment of the condition.
Causes of Hiatal Hernia
The development of a hiatal hernia is often linked to several risk factors and causes:
Women and individuals over the age of 50 are more likely to develop this condition.
Those who are overweight have an increased risk, as excess weight can put pressure on the abdomen and contribute to the formation of a hiatal hernia.
A weak spot in the diaphragm, the muscle that separates the chest cavity from the abdomen, can also lead to a hiatal hernia.
Several factors can contribute to the weakening of these tissues, including scar tissue, injuries, surgeries, congenital disabilities, and cumulative damage from stress and strain.
For instance, trauma or surgical procedures involving the diaphragm can create areas of weakness that make it easier for the stomach to push through the diaphragmatic hiatus.
Consistent high pressure on the abdominal muscles, such as from heavy lifting or chronic straining, can also lead to the development of a hiatal hernia. Recognizing these causes aids in both preventing and managing the condition effectively.
Diagnosis Methods for Hiatal Hernias
Diagnosing a hiatal hernia is a critical step in managing the condition effectively. One of the preferred methods for diagnosis is a barium swallow study, where the patient drinks a chalky liquid that coats the esophagus and stomach, making them visible on X-rays. However, this method has its limitations, such as the potential to miss small or intermittent hernias and radiation exposure. Endoscopy may also have difficulty visualizing a large hiatal hernia, especially those involving organo-axial rotation of the stomach, making barium swallow X-ray particularly useful for identifying large hiatal hernias.
Physical exams can provide initial indications of a hiatal hernia, but are often supplemented with imaging techniques for a more accurate diagnosis. A physical exam can be a helpful first step in this process. High-resolution manometry is another effective method used to rule out motility disorders that may mimic a hiatal hernia.
Additionally, ultrasonography can diagnose gastroesophageal reflux with high sensitivity, providing a comprehensive understanding of the condition. These diagnostic methods ensure that the appropriate treatment plan is developed.
Non-Surgical Treatment Options
Managing a sliding hiatal hernia doesn't always require surgery. Many individuals find effective relief through non-surgical means such as lifestyle modifications and medications. Medical treatment is typically the first-line approach for managing hiatal hernia symptoms, with surgery reserved for cases where medical treatment does not provide adequate relief. These approaches can significantly alleviate symptoms and reduce the risk of recurrence, making treatment of hiatal hernia a viable option for many.
Managing hiatal hernia symptoms and preventing further complications involves maintaining a healthy weight, making dietary changes, and engaging in regular exercise.
Lifestyle Changes
Lifestyle changes can be highly effective in managing the symptoms of a hiatal hernia. These include:
Eating smaller, more frequent meals can reduce the pressure on the stomach and alleviate symptoms.
Avoiding specific foods that trigger heartburn, such as fried items, alcohol, and spicy foods.
Adopting a diet rich in lean meats, non-citrus fruits, and whole grains can help manage symptoms effectively.
Maintaining a healthy weight is another critical factor in managing hiatal hernia symptoms. Excess weight can increase pressure on the abdomen, exacerbating symptoms and increasing the risk of recurrence. Regular exercise not only helps in weight management but also strengthens abdominal muscles, providing better support for the digestive system.
These lifestyle changes can make a significant difference in symptom relief and overall quality of life.
Medications
Medications play a vital role in the non-surgical treatment of hiatal hernias. Proton pump inhibitors (PPIs) are commonly used to:
Decrease stomach acid production, which can significantly alleviate GERD symptoms linked to hiatal hernias
Reduce acid reflux
Prevent damage to the esophagus. These effects offer substantial symptom relief.
Surgical Treatments for Hiatal Hernias
When non-surgical treatments are insufficient, surgical options become necessary. Various surgical techniques are available to treat hiatal hernias, each with its specific approach and benefits. Elective repair may be recommended for patients with asymptomatic or minimally symptomatic hernias to prevent complications such as strangulation or perforation. Hiatal hernia repair encompasses a range of surgical procedures designed to restore normal anatomy and function. Minimally invasive approaches, such as laparoscopic repair, are increasingly preferred due to their benefits in recovery and outcomes.
Understanding these surgical treatments is crucial for effective management and long-term relief from hiatal hernia symptoms.
Laparoscopic Nissen Fundoplication
Laparoscopic Nissen fundoplication is a standard and effective surgical procedure for treating hiatal hernias. This minimally invasive laparoscopic surgery technique involves moving the stomach and lower esophagus below the diaphragm and tightening the diaphragm opening. The procedure often leads to shorter recovery times and reduced postoperative pain compared to traditional open surgery. Laparoscopic paraesophageal hernia repair is another minimally invasive technique explicitly used for paraesophageal hernias, offering similar benefits in terms of recovery and outcomes.
One of the significant advantages of this method is its ability to minimize the chances of dysphagia and reduce gas bloating significantly. This surgical technique addresses the root cause of acid reflux, offering long-term relief and fewer complications, including surgical endoscopes.
Belsey Fundoplication
The Belsey fundoplication technique is another surgical method used in the treatment of hiatal hernias. This procedure involves a 270° wrap around the esophagus, designed to enhance its efficacy. The specific design of the 270° wrap helps in decreasing postoperative gas bloating, a common issue with other surgical techniques.
This approach is efficient in managing acid reflux and related symptoms, providing significant relief for patients. By addressing the structural issues that cause hiatal hernias, the Belsey fundoplication offers a robust solution with lasting benefits.
Hill Repair
The Hill repair method focuses on securing the stomach's cardia to enhance the lower esophageal sphincter's support. By anchoring the stomach's cardia, this technique provides a robust antireflux mechanism, reducing the risk of paraesophageal hernia repair and hernia recurrence.
This surgical repair approach offers an effective solution for long-term management of hiatal hernias.
Magnetic Sphincter Augmentation
Magnetic sphincter augmentation is a modern technique that utilizes small magnetic beads to create a barrier against acid reflux. This method is particularly effective in reducing GERD symptoms, providing significant relief with fewer complications compared to traditional surgical options, especially by enhancing the function of the lower esophageal sphincter.
The magnetic beads create a barrier at the gastroesophageal junction, preventing stomach acid from flowing back into the esophagus. This technique has shown lower rates of complications, making it a promising option for those seeking surgical treatment for hiatal hernias.
Postoperative Care and Recovery
Postoperative care is crucial for a smooth recovery after hiatal hernia surgery. Patients may experience dysphagia, which is usually temporary and resolves within a few weeks. Gas bloating is another common side effect, particularly after laparoscopic Nissen fundoplication. Other postoperative complications can include issues such as recurrence, Infection, or erosion, and careful monitoring and follow-up are essential to address these complications promptly.
Patients typically stay in the hospital for one to two days post-surgery. Post-surgery care recommendations include:
Follow a liquid diet for about three weeks due to initial swelling in the esophagus.
Engage in walking and normal activities immediately after surgery.
Avoid heavy lifting to prevent complications.
Contact the surgeon if fever or persistent nausea occurs.
Preventing Hiatal Hernia Recurrence
Preventing the recurrence of a hiatal hernia involves a combination of surgical techniques and lifestyle modifications. Surgical methods aim to approximate the diaphragm crura, enhancing stability and reducing the chances of recurrence.
Avoiding activities that increase abdominal pressure, such as heavy lifting or chronic straining, is crucial in preventing recurrence. Maintaining a healthy weight, making dietary changes, and regular follow-up care are essential components of a comprehensive prevention plan.
Summary
In summary, understanding the symptoms, causes, and treatment options for hiatal hernias is crucial for effective management and recovery. From lifestyle changes and medications to advanced surgical techniques, there are various ways to manage this condition. By taking proactive steps and seeking appropriate medical care, individuals can find relief and improve their quality of life. Remember, knowledge is power, and being informed is the first step towards effective treatment and prevention of hiatal hernias.
Frequently Asked Questions
What are the common symptoms of a hiatal hernia?
The common symptoms of a hiatal hernia include heartburn, belching, chest pain, difficulty swallowing, and fatigue. If you are experiencing these symptoms, it may be advisable to seek medical attention.
What causes a hiatal hernia?
A hiatal hernia is caused by factors such as age, being overweight, a weak diaphragm, injuries, and chronic straining. Addressing these risk factors can help prevent their occurrence.
How is a hiatal hernia diagnosed?
A hiatal hernia is diagnosed through several methods, including barium swallow studies, physical examinations, high-resolution manometry, and ultrasonography. These techniques help healthcare professionals accurately assess the condition.
What non-surgical treatments are available for hiatal hernias?
Non-surgical treatments for hiatal hernias primarily focus on lifestyle modifications, including dietary changes and weight management, along with the use of medications such as proton pump inhibitors. Implementing these strategies can effectively alleviate symptoms without the need for surgical intervention.
What are the surgical options for treating a hiatal hernia?
Laparoscopic Nissen fundoplication, Belsey fundoplication, Hill repair, and magnetic sphincter augmentation are effective surgical options for treating a hiatal hernia. These procedures aim to restore proper function and alleviate symptoms associated with the hernia.
"Thank you for joining me today on The Gut Whisperers.
We've seen how hiatal hernia symptoms can start as early as infancy — from spit-ups, ear infections, and chronic cough — and evolve into reflux, chest pain, and swallowing difficulties in adolescents. The important takeaway is this: early recognition and treatment can prevent years of discomfort and help children return to living whole, healthy lives.
If you or your child is experiencing symptoms, don't wait — talk to a specialist and explore the treatment options we discussed today, from lifestyle changes to advanced surgical techniques.
A special thanks to our sponsors:
Laguna by Andrés Spinetti, a breathtaking tribute to the Laguna Madre, is available now at carenowonline.com/products/laguna-pioner.
"Request your 10 red flag of newborn in infants here"
The Pediatric Gastroenterology Clinic of South Texas is dedicated to helping families find real answers and relief. Visit us at pgcost.com or call (956) 682-2244.
I'm Dr. Nelson Spinetti, and this has been The Gut Whisperers. Until next time, remember: listen to your gut — it's always trying to tell you something."